Stories from the front lines: ICU doctor urges public to help them “flatten the curve” on the coronavirus by staying home
03/29/2020 / By Zoey Sky
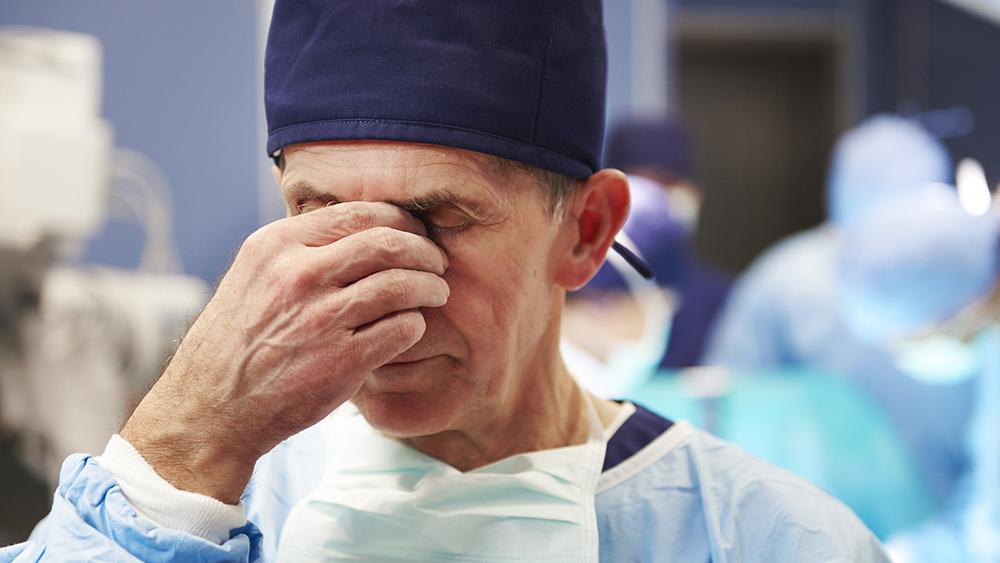
In a bid to combat the COVID-19 pandemic, health care workers are on the front lines looking after infected patients and sharing guidelines on how to effectively control the spread of the novel coronavirus. It’s a ceaseless job, but an ICU doctor in Honolulu says that it’s an honor for them to care for the sick.
However, it’s also a terrifying task because there is currently no cure for COVID-19.
Battling coronavirus
Spreading throughout the U.S., COVID-19 has reached the ICU. Dr. Philip A. Verhoef, an ICU doctor and a clinical assistant professor of medicine at the University of Hawaii at Manoa John A. Burns School of Medicine in Honolulu, talks about life in the ICU as he cares for COVID-19 patients.
Verhoef says his role shifting from trying to prevent the spread of the virus to treating infected patients has opened his eyes to the gravity of the situation. It also presented him with a dilemma: What should a doctor do when there are too many patients and not enough medical staff or equipment?
The COVID-19 pandemic is challenging how governments and institutions like hospitals handle this kind of situation.
Working on the front lines
Health care professionals have become on edge when they feel the need to cough, which was considered normal until the pandemic. Now, coming down with a cough or experiencing flu-like symptoms is enough to make even experienced doctors like Verhoef panic.
In a pre-pandemic world, Verhoef would have only used a mask for certain patients and changed it every time he visited a different patient room. These days, Verhoef limits his use of masks to one per day. And if he uses a face shield, it must be wiped it down and reused whenever possible.
On days when Verhoef must care for COVID-19 patients, he changes into hospital scrubs when he arrives at the hospital. And before he leaves, Verhoef changes out of those scrubs, showers and wipes down items like his glasses, phone and other belongings with sanitizing wipes to protect his children at home. Verhoef’s 70-year-old in-laws also live with them, which means he must be twice as careful while sanitizing his belongings.
Verhoef shares that when caring for those with respiratory failure who exhibit COVID-19 symptoms, conscious patients typically report feeling like they’re drowning. Doctors force these patients to breathe with the smallest amount of air possible.
Most of the time, patients who have breathing difficulties must go into an induced coma. Doctors may also need to use medication to sedate them. The patients also require a breathing tube, which is painful and uncomfortable, and prevents them from talking.
While caring for patients with COVID-19, Verhoef shares that flipping patients onto their stomachs is effective. At least once or twice a day, nurses, respiratory therapists and physicians turn comatose patients over and back. Patients are fed via additional tubes in the mouth or nose, and medications are infused to optimize the support of every organ in a patient’s body.
Despite these techniques, Verhoef and his fellow health care professionals are worried about making mistakes that can harm a patient or cost someone their life.
Verhoef shares that he feels overwhelmed while thinking of how they are now tasked with looking after the wave of critically ill COVID-19 patients they’re anticipating.
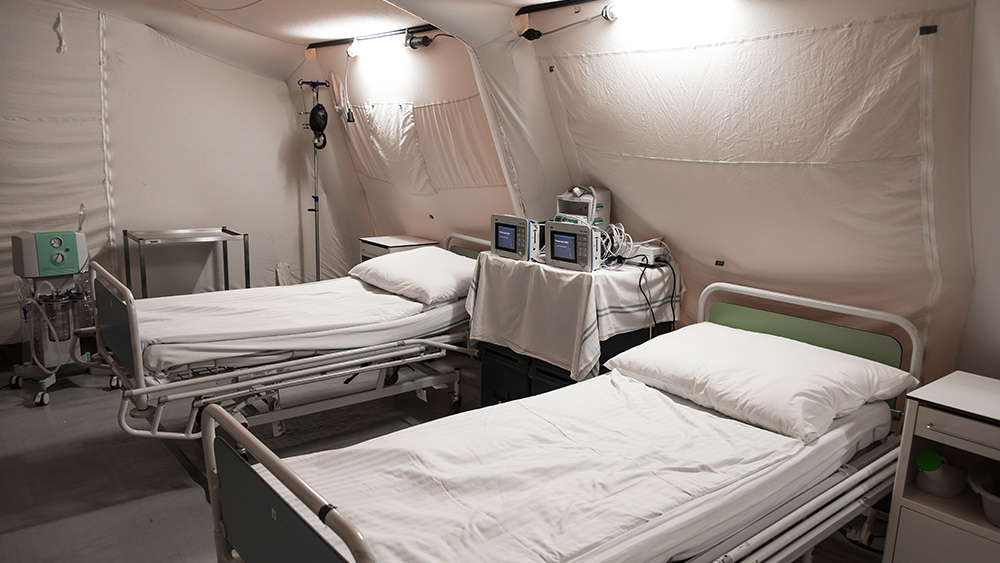
One model suggests that the number of expected sick patients will exceed the number of hospital beds in Hawaii between April 20 and May 10, which will have devastating consequences.
To prepare for this estimated wave of patients, Verhoef says that hospitals must have enough personal protective equipment to keep their staff safe. Unfortunately, Verhoef and his colleagues only have at least two weeks’ worth of supplies.
Verhoef adds that they could deplete the entire supply of ventilators in Hawaii. The wait for new ventilators can take several weeks.
Help us “flatten the curve” on coronavirus, pleads doctor
Hospitals must reevaluate the roles of health care providers. For example, outpatient primary care doctors may be recruited to work in the hospital, while hospitalists or doctors who normally care for hospital patients who are not critically ill may be needed in the ICU.
Verhoef explains that intensivists like him are usually involved in various aspects of care for ICU coronavirus patients. Intensivists perform procedures, manage ventilators and talk to families.
But there is a limited number of ICU doctors in hospitals, and it is impossible to have one of them looking after a patient 24/7.
Ironically, Verhoef says he may have the least amount of patient contact since he’s leading teams of hospitalists that are now looking after many critically ill patients.
Hospitals must also establish protocols for rationing the limited resources that they have. Because of the pandemic, doctors might have to make difficult decisions.
What if there were 10 patients who needed a ventilator each, but the hospital only had five? Verhoef urges for a rational process for “literally deciding who will live and who will die.”
Verhoef believes the worst part of trying to control the spread of the coronavirus is the fact that they’re dealing with a new disease.
COVID-19, according to Verhoef , “is more severe, it lasts longer, it is unpredictable, it may impact the heart and, most important, there is no cure.”
How you can help
Despite fearing for their own health and that of their loved ones, health workers like Verhoef and other medical staff remain at the forefront of the global fight against the coronavirus.
Verhoef asks the public to help “flatten the curve,” on COVID-19, which can give health workers a better chance of looking after every patient who falls ill.
In epidemiology, the curve is “the projected number of new cases over a period of time.”
“Flattening the curve” doesn’t guarantee that the spread will grind to a halt. What it does mean is that instead of a sudden uptick in new cases, which is overwhelming medical facilities around the world, there would just be a gradual increase in the number of patients infected, which is less likely to overburden the health care system.
Here are some things you can do:
- Wash your hands regularly and thoroughly.
- Avoid touching your eyes, nose and mouth to prevent contracting any viruses.
- Practice social distancing.
- Seek medical care immediately if you experience symptoms like a fever, cough or difficulty breathing.
Flattening the curve can help stagger the number of new cases over a longer period, which gives the infected patients access to better healthcare. Because of this, many countries are implementing preventive methods like social distancing, restricting non-essential travel and giving workers the option to work from home.
Help frontliners like Verhoef by doing your part. Read the latest news on COVID-19 at Pandemic.news.
Sources include:
Submit a correction >>
Tagged Under:
chaos, coronavirus, covid-19, crisis, disaster, doctors, hand washing, health workers, healthcare system, Hospitals, hygiene, ICU, infections, medical facilities, medical staff, outbreak, pandemic, panic, prevention, Public Health, social distancing, superbugs, viral infection, virus
This article may contain statements that reflect the opinion of the author
RECENT NEWS & ARTICLES
Infections.News is a fact-based public education website published by Infections News Features, LLC.
All content copyright © 2018 by Infections News Features, LLC.
Contact Us with Tips or Corrections
All trademarks, registered trademarks and servicemarks mentioned on this site are the property of their respective owners.